Article reviewed and approved by Dr. Ibtissama Boukas, physician specializing in family medicine
A flavectomy is the surgical removal of the yellow ligament. This operation reduces the pressure exerted by a hypertrophied or dysfunctional ligamentum flavum in the spinal canal, and thus reduces pain.
This article explains everything you need to know about flavectomy.
Definition and anatomy
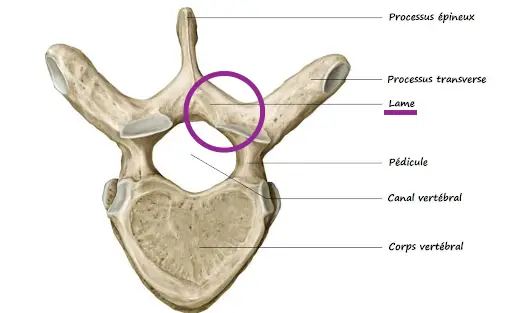
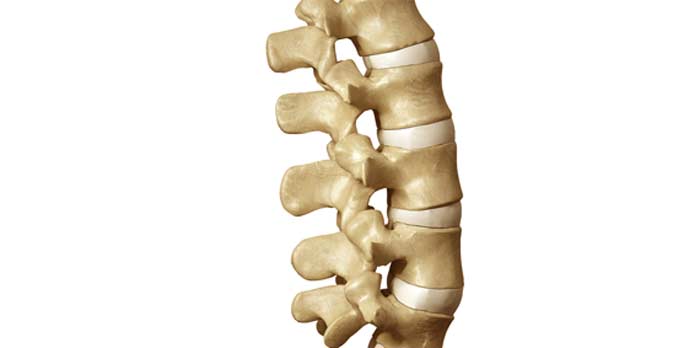
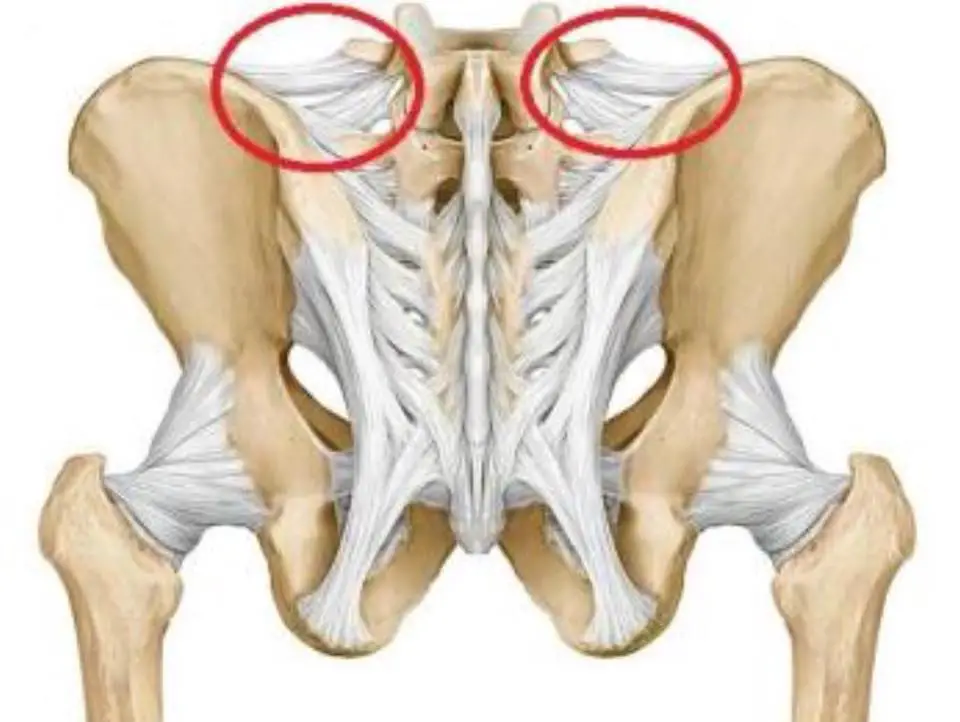
The yellow ligaments are ligaments that run between the laminae of the vertebrae full spine. They are found all along the spine (on both sides), from the vertebrate cervical C2, up to vertebra S1.
They have elastic fibers that allow them to contract naturally, in a way. Therefore, they help in the extension of the spine and maintaining the upright posture. In addition, the yellow ligaments prevent excessive flexion of the spine by their tension.
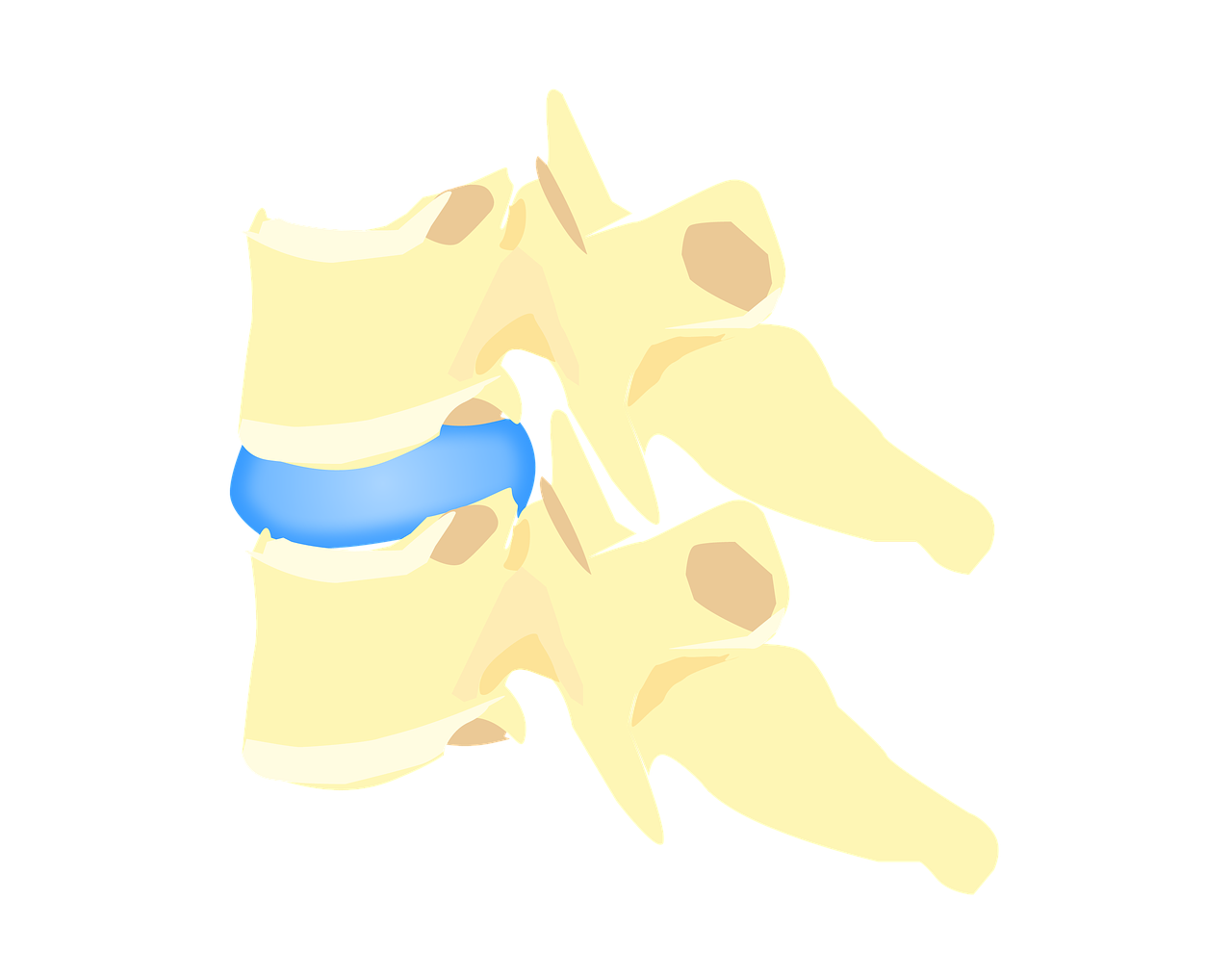
The yellow ligament can undergo degeneration with age, or after repeated trauma. Under these circumstances, it loses elastic capacity, and increases in thickness. Due to hypertrophy (called yellow ligament hypertrophy), other related structures may be irritated, pinched or even compressed. We think in particular of the spinal cord and emerging nerve roots.
This can lead to potentially serious spinal injuries, such as cauda equina syndrome, narrow lumbar canal, or a spinal cord compression.
Procedure
A flavectomy is performed to decompress the spinal canal. Whether due to hypertrophy of the yellow ligament, or herniated disc forcing the yellow ligament to sink into the Spinal canal, excision of this ligament will release pressure on the spinal cord and spinal nerves.
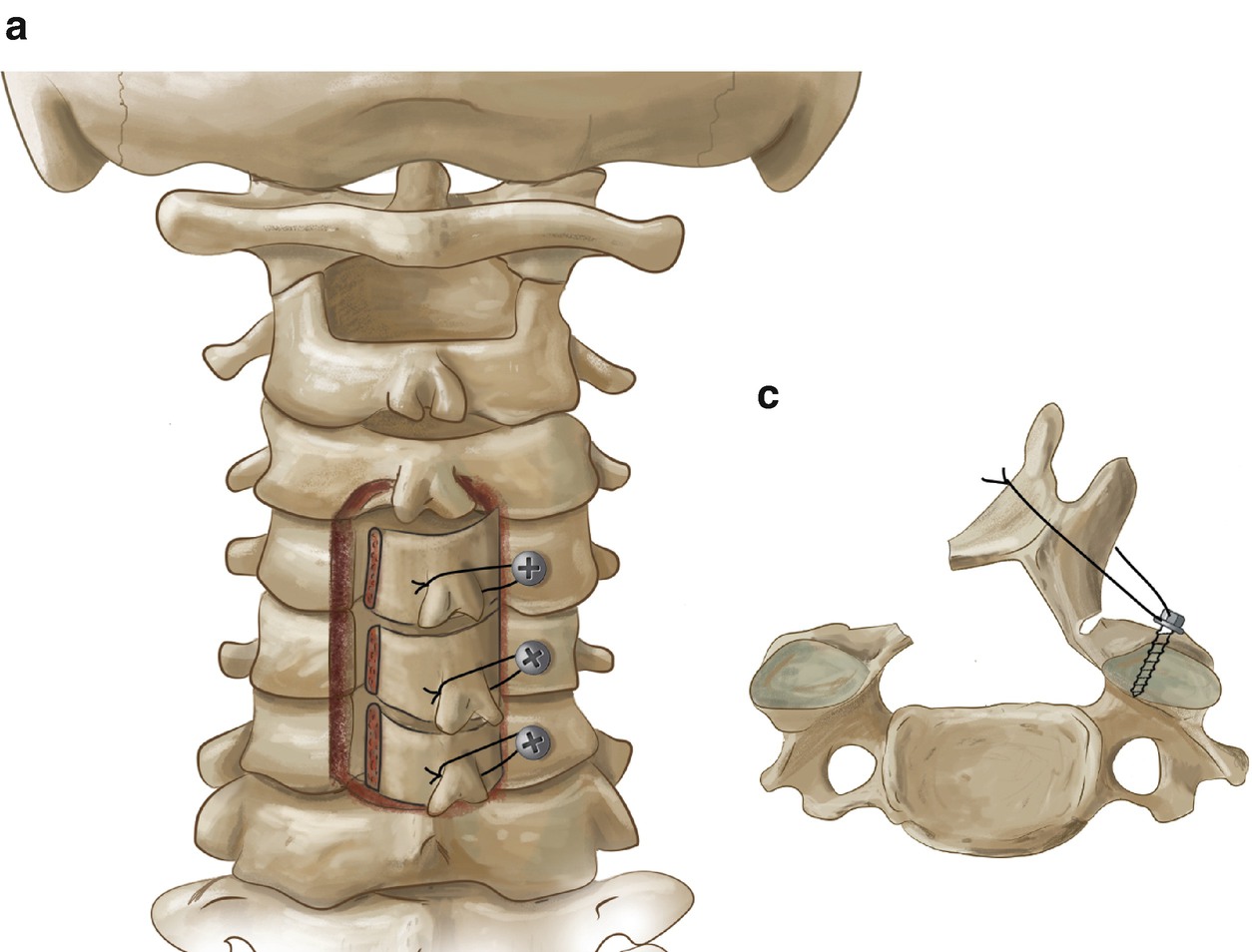
Flavectomy is sometimes associated with laminectomies to better free the spinal canal.
Other types of decompressive surgery
Alternatives to flavectomy include:
- Laminoplasty
- Laminectomy
- Discectomy
- Corpectomy
- Foraminotomy
- Arthrodesis
It should be noted that the optimal surgical technique for treating the spinal compression or nerve roots remains controversial. One approach is not necessarily superior in all circumstances, and the best option will depend on patient-specific anatomical and symptomatic factors.