Article reviewed and approved by Dr. Ibtissama Boukas, physician specializing in family medicine
What is kyphoplasty, and in which cases is this operation indicated? Is she sure? This article tells you everything you need to know about this surgery.
Definition
La kyphoplasty is a set of minimally invasive surgical techniques (i.e. access is through several small incisions and the part of the spine to be operated on is not revealed) which consists of repairing a spinal column damaged.
It is one of the treatment techniques for vertebral fractures often caused by osteoporosis.
In healthy patients, a serious accident can, as a rare consequence, cause a vertebral fracture.
In patients with osteoporosis, vertebral fracture can occur in everyday life. Something as trivial as tripping on the stairs while carrying a bag, sneezing or coughing can cause a spinal fracture[1].
The operation of vertebroplasty ou kyphoplasty is the fruit of a long medical journey. For decades, kyphoplasty has been performed as an open spine surgery to increase the volume of the fractured vertebra and relieve pain. However, since 1984, this procedure has been used as a minimally invasive operation: percutaneous vertebroplasty has become a standard operation following an osteoporotic brain fracture.[2].
Indication (3)
Tumors
The first indications for vertebral cementoplasty concerned symptomatic vertebral angioma. They then spread to benign (vertebral hemangioma) or malignant (metastases, myeloma) tumor lesions.
Only 3% of vertebral fractures are of malignant origin. They are a significant source of morbidity in patients with metastatic solid vertebral tumors or malignant myeloma with a poor prognosis. These fractures are common and are generally painful.
Their treatment is often palliative (analgesics, radiotherapy, corset) and sometimes etiological (chemotherapy, etc.). A cementoplasty can be proposed in case of painful vertebral localization without sign of compression.
osteoporosis
It is estimated that 85% of vertebral fractures are of osteoporotic origin. Their annual incidence is estimated at more than 700000 in the United States and 450000 in Europe and yet only a third of them would be diagnosed. They are twice as common in women after menopause. They can occur spontaneously or after minimal trauma.
The conventional treatment of osteoporotic vertebral compression is based on analgesics associated or not with a corset. A period of bed rest in the acute phase may be necessary followed by early mobilization with physiotherapy. Comprehensive management of osteoporosis by the rheumatologist or general practitioner must be systematically associated (bone densitometry, bisphosphonates, etc.).
In osteoporotic pathology, cementoplasty is never performed in an emergency but there is currently no consensus on this subject. In our practice, we offer it in the event of failure of well-conducted medical treatment for at least 1 month, with radio-clinical correlation with scintigraphy or MRI.
In a series of 254 patients with an osteoporotic vertebral fracture treated with kyphoplasty, Majd reported an immediate reduction in pain after the procedure in 89% of cases, with in 63% of cases a restoration of at least 20% of the vertebral height.
Fractures in the young subject
“Stand alone” kyphoplasty seems to us to be an interesting alternative to traditional treatments for compression fractures (type A of Magerl) of the thoraco-lumbar hinge in the absence of neurological signs. Unlike the corset, it allows a significant reduction in traumatic vertebral kyphosis.
This lasting restoration of the anatomy of the vertebral body is directly correlated with a good functional result, as shown in the 2008 Western Orthopedic Society round table.
After appropriate information, we offer young patients kyphoplasty, because it allows correction of traumatic vertebral deformity while preserving the complications of corset and open surgery.
Kyphoplasty procedure (4)
- Kyphoplasty or vertebroplasty is performed while the patient is lying on their stomach.
- You can choose between local or general anesthesia.
- A skin incision of no more than 1 cm is made to serve as a surgical opening.
- Insertion of a tube (working channel) into the fractured vertebral bone under X-ray guidance.
- A thin tube with an inflatable balloon (called a buffer balloon) is guided into the damaged vertebral bone.
- The balloon is inflated until the original height of the fractured vertebra is restored.
- After sufficient cavity has been created, the balloon is deflated and removed.
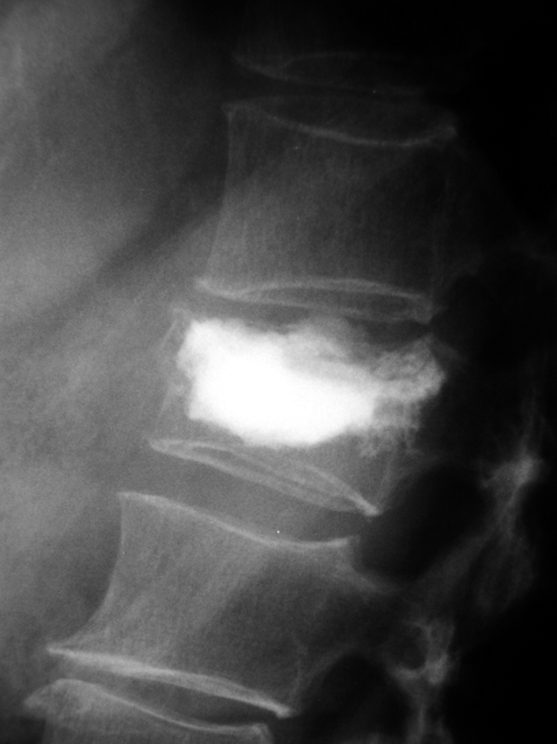
- Bone cement or silicone material is injected into the cavity.
- This bone cement hardens within 10 minutes. It fixes fractured particles of bone, effectively acting as an internal plaster.
Complications
The complications of kyphoplasty or simple vertebroplasty are well known. They are, on the whole, infrequent and operator-dependent.
Cement leaks can occur in the epidural space, foramina, pre- or latero-vertebral soft tissues, adjacent intervertebral discs, and peri-vertebral vessels. Epidural or foraminal leaks can be responsible for neighboring nerve compressions, but, fortunately, this complication is exceptional. Small asymptomatic venous leaks are common and are explained by the density of the perivertebral venous plexuses.
Distant cement vascular migrations are rarer, but may be underestimated. Cement micro-emboli in the pulmonary vasculature are not uncommon if a chest CT scan without injection is systematically done after vertebroplasty performed with cements of low or medium viscosity.
Studies comparing vertebroplasty and balloon kyphoplasty suggest that the latter carries less risk of leakage. Finally, the use of very viscous cements is recommended by some to reduce this risk of leakage.[5].
Conclusion
Kyphoplasty is one of the techniques for treating vertebral fractures often caused by osteoporosis.
Osteoporosis should be treated first; For The conventional treatment of osteoporotic vertebral compression relies on analgesics associated or not with a corset.
A period of bed rest in the acute phase may be necessary followed by early mobilization with physiotherapy.
Comprehensive support for osteoporosis by the rheumatologist or the general practitioner must be systematically associated with it. We have fewer complications in vertebral cementoplasty which can be explained by the low pressure injection of cement into a preformed cavity during kyphoplasty.
Resources
[1] Gelenk-Klinik Orthopedic Clinic; ISO 9001:2008 2008 certified quality
[2] IDEM
[3] P. PRIES; Kyphoplasty and vertebroplasty; Elsevier Masson SAS; 2013; P 221-234
[4] Lindsay R, Silverman SL, Cooper C, and al. Risk of new vertebral fracture in the following year
has a fracture. JAMA. 2001;285(3):320-3
[5] Bull. Acad. Natle Med. City of Kyiv, Ukraine, 201, nos 1-2-3, 395, session of February 28, 2017