Article reviewed and approved by Dr. Ibtissama Boukas, physician specializing in family medicine
Spondylodesis is a surgical procedure to fuse together two (or more) vertebrae of the spine. It is used when conventional approaches fail in order to relieve pain and restore quality of life to the affected patient.
When to consider this operation? How is it going? Are there any risks? How to resume normal activities after surgery? This article answers all your questions about spinal fusion.
Definition
Also called arthrodesis, spinal fusion (spondylodesis) is a surgical procedure in which two or more vertebrae are permanently fused together to form strong bone, with no gaps in between. Although it can be performed anywhere on the spine, it mainly involves the cervical vertebrae (cervical arthrodesis) and lumbar (lumbar arthrodesis).
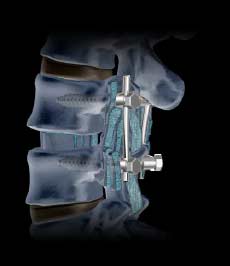
During surgery, your surgeon places bone (or bone-like material) in the space between two spinal vertebrae. Metal plates, screws, and rods are also used to hold the vertebrae together, so they can heal into one solid unit.
Indications
Spinal fusion permanently connects two or more vertebrae in your spine to improve stability, correct deformity, or reduce pain. Your doctor may recommend spinal fusion to treat:
Spinal deformities
Spinal fusion can help correct spinal deformities, such as a lateral curvature of the spine (Scoliosis).
Weakness or instability
Your spine can become unstable if there is abnormal or excessive movement between two vertebrae. This is a common side effect of severe arthritis of the spine. Spinal fusion can be used to restore spinal stability in such cases.
Herniated disc
Spinal fusion can be used to stabilize the spine after a damaged (herniated) disc has been removed. To know everything about the herniated disc, see the following article.
Procedure
First, preparation before surgery may involve shaving off the hair at the surgical site and cleaning the area with a special soap or antiseptic. Additionally, the surgical team may order monitoring for any unhealthy bacteria in your nose by taking a swab sample. Tell your doctor about the drug treatments you are undergoing, this is very useful if you have to stop taking a type of medicine.
Surgeons perform a spinal fusion while you are under general anesthesia, so you are unconscious during the procedure. Surgeons have developed a variety of techniques to perform spinal fusion surgery. The technique your surgeon uses depends on the location of the vertebrae to be fused, the reason for the spinal fusion, and, in some cases, your general health and body shape.
Typically, the procedure includes the following:
Cut: To access the vertebrae to be fused, the surgeon makes an incision in one of three places: in your neck or back directly above your spine, on either side of your spine, or in your abdomen or throat so that your surgeon can access the spinal columns from the front.
Bone graft preparation: Bone grafts that actually fuse two vertebrae together can come from a bone bank or from your own body, usually from your pelvis. If your own bone is used, the surgeon makes an incision above your pelvic bone, removes a small portion of it, and then closes the incision.
Fusion : To permanently fuse the vertebrae together, the surgeon places bone graft material between the vertebrae. Plates, screws, or metal rods may be used to help hold the vertebrae together while the bone graft heals.
In some cases, some surgeons use a synthetic substance instead of bone grafts. These synthetic substances help promote bone growth and accelerate vertebral fusion.
Risks and complications
Spinal fusion is generally a safe procedure. But as with any surgery, spinal fusion carries the potential risk of complications.
Potential complications include:
- Infection
- Poor healing
- Bleeding
- Blood clots
- Injury to blood vessels or nerves in and around the spine
- Pain at bone graft harvesting site
Recovery and rehabilitation
A hospital stay of two to three days is usually required after spinal fusion. Depending on the location and extent of your surgery, you may experience some pain and discomfort, but the pain can usually be well controlled with medication.
After you go home, contact your doctor if you have any signs of infection, such as:
- Redness, tenderness or swelling
- Wound drainage
- Frissons
- Fever above 38°C
It may take several months for the affected bones in your spine to heal and fuse together. Your doctor may recommend that you wear a brace for a while to keep your spine properly aligned. Physical therapy (physiotherapy) can teach you how to move, sit, stand, and walk in a way that keeps your spine properly aligned.
Recovery
Recovery after spinal fusion surgery can be slow and painful, and the time it takes to feel like yourself again depends on a variety of factors:
- your age
- your health status
- the extent of the procedure performed.
- the type of graft used (It may take longer to recover from a pelvic autograft procedure than one that uses a local autograft or allograft).
Older people or those who have had more extensive procedures can take four to six months to recover. Younger patients may bounce back faster, but should still expect it to take them four to six weeks to return to office work, even longer for physical labor.
Remember to schedule a post-surgical follow-up appointment within two to four weeks of your surgery, or as instructed.
Physical activity
For the first two weeks after surgery, you should limit going up and down stairs to once a day, take short walks, and not sit for more than 20 minutes at a time.
You also won't be allowed to drive until cleared by your healthcare provider and should avoid car trips longer than 30 minutes without taking a break to stretch your legs.
Avoid housework, carrying anything over 10 pounds (including children), or lifting anything above your head until your incision heals.
If you have been fitted with a back brace or support after spinal fusion surgery, it is generally recommended to wear it while sitting and walking, but it may not be necessary to wear it while sleeping. depending on your condition.
Follow all instructions from your medical team to resume normal activity and exercise, including sexual activity.
My Healing
You will need to keep the incision dry for the first five to seven days and cover it with plastic wrap when bathing. The dressing will probably peel off on its own after seven to 10 days.
It is normal for the incision to be red, numb, or painful as it heals, but watch carefully for signs of infection. You should also watch for symptoms of blood clots:
- swelling below the knee
- tenderness or redness around the knee
- calf pain
Blood clots can be dangerous if they cross the bloodstream and settle in the lungs.
Pain management
Recovery after spinal fusion surgery can be painful, and you'll likely leave the hospital with a prescription for opioid painkillers, such as OxyContin (oxycodone) or Percocet (oxycodone with acetaminophen).
Although opioids are very effective pain relievers, they are addictive and should be used sparingly. Side effects of opioids can also be significant and include nausea, vomiting, constipation, urinary retention, drowsiness, impaired thinking ability, and poor respiratory function.
Nonsteroidal anti-inflammatory drugs and over-the-counter painkillers such as Tylenol (acetaminophen) and Advil (ibuprofen) can also be used to treat post-surgical pain. Many health professionals recommend alternating the dosage between the two. However, Percocet also contains acetaminophen and should not be taken with Tylenol as liver damage may occur.
Specifically, if you experience any of the following symptoms, call your healthcare professional:
- Chills or fever of 40°C or more
- No more pain in the operated area
- The incision is warm to the touch with more redness and swelling
- Drainage from the incision, especially if the drainage is green, yellow, or foul-smelling
- Loss of sensation or change in sensation in your arms (if you had neck surgery) or your legs and feet (if you had lower back surgery)
- Swelling in the legs
- Calf pain
- Back pain that gets worse and does not improve with rest and painkillers
- Difficulty urinating and controlling your bowel movements
Also, head to the emergency room if you experience chest pain or shortness of breath, as this may be a sign that a blood clot has traveled to the lungs.
My name is Anas Boukas and I am a physiotherapist. My mission ? Helping people who are suffering before their pain worsens and becomes chronic. I am also of the opinion that an educated patient greatly increases their chances of recovery. This is why I created Healthforall Group, a network of medical sites, in association with several health professionals.
My journey:
Bachelor's and Master's degrees at the University of Montreal , Physiotherapist for CBI Health,
Physiotherapist for The International Physiotherapy Center