Article reviewed and approved by Dr. Ibtissama Boukas, physician specializing in family medicine
Also called the cervical spine, the cervical spine forms the region of the neck. Its function is essential, and this region can be the site of several pathologies.
What is the cervical spine, and what are the most common symptoms encountered with a neck problem? When should you worry? What treatments to consider?
This popular article explains everything you need to know about this part of the spine.
Definition and anatomy of the cervical spine
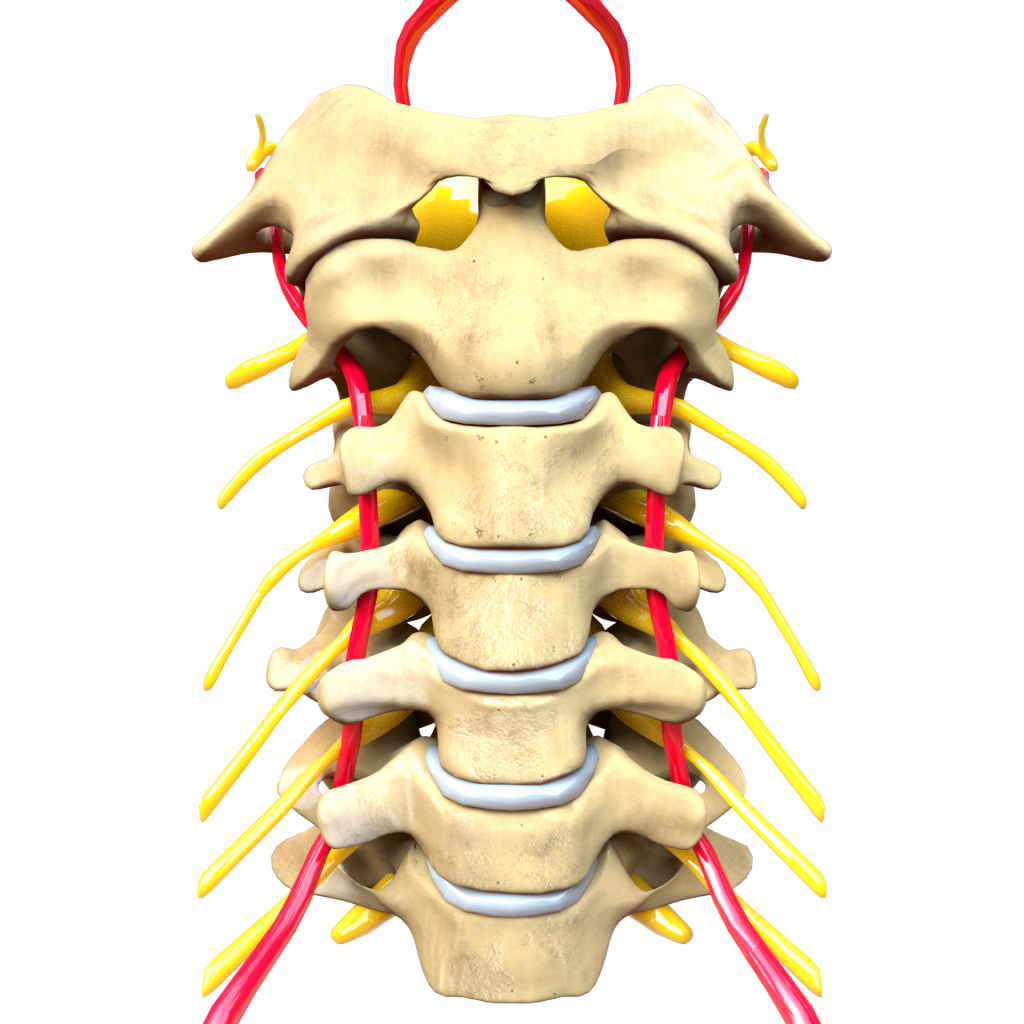
The cervical spine is part of the spine. It is made up of 7 bones, or vertebrae, numbered from C1 to C7. The vertebrae are separated from each other by intervertebral discs. These discs help absorb shock and also facilitate neck movement.
A vertebra is made up of a vertebral body at the front, and a bony arch at the back. The space between the body and the posterior arch forms a channel that runs the entire length of the back. It is called the spinal canal (or spinal canal).
It is through this space that the spinal cord and spinal nerves pass (via openings called foramens on either side of the spine). These nerves will travel to the upper limbs to provide sensation and movement.
The cervical spine is supported in a series of muscles and ligaments attached to the vertebrae. One of their main roles will be to protect the spinal cord and the vasculo-nervous bundle (blood vessels and nerves) around the neck.
Pathologies of the cervical spine
The cervical spine can be the site of several pathologies. These can be traumatic (after an accident) or appear gradually.
Essentially, any damage to the discs, muscles, ligaments, vertebrae or joints in the neck can cause pain and other dysfunctions.
Among the most common pathologies are:
- Cervical arthritis
- Reverse curvature (or straightness of the cervical spine)
- Degenerative disc disease
- Cervical hernia
- Cervico brachial neuralgia
- Polyarthrite rhumatoïde
- whiplash and cervical sprain
- Arnold's neuralgia
Symptoms of the disease
Obviously, the symptoms observed will depend on the pathology. To know the symptoms caused, it is necessary to understand the anatomical and physiological role of the irritated structure.
The symptoms will also depend on the individual concerned, as the body's ability to adapt and tolerance to pain is different for everyone.
For example, nerve damage could cause radiating pain, as well as numbness and tingling in the upper limbs.
Ligament damage could cause local pain aggravated by movements putting tension on the ligaments concerned.
Muscle damage could cause local inflammation, and limit movements involving contraction of irritated muscles.
Vascular damage could indirectly affect vision or hearing.
In short, here is a list of symptoms often associated with cervical spine disorders:
- Pain in the neck
- Headache-like pain referred to the head (on one or both sides)
- Pain radiated to the upper limb (shoulder, elbow, wrist, fingers)
- Numbness and tingling (ants in hands)
- Burning sensation
- Feeling of weakness
- Neck cracks
- Dizziness
- Acouphènes
- Vision disorders
- nausea
Physical examination
When consulting a health professional for a cervical spine disorder, he will generally follow a structure to clarify the situation, and then issue one (or more) diagnostic hypothesis (s).
The examination will most often begin with a medical questionnaire where you will be asked questions about your health, your pain and other symptoms, the impact on your daily life, your goals, etc.
Then, the professional will do a clinical examination. The primary objective is to exclude serious damage (such as cancer, or damage to the spinal cord) that would constitute a medical emergency.
This notably involves neurological tests (Clonus, Babinski, reflexes, sensation, muscle strength, coordination, vision, etc.).
Once serious damage has been ruled out, cervical spine movements such as flexion, extension, rotations and lateral tilts will generally be assessed. This will give us information about the irritated structures.
Other more advanced clinical tests will help clarify the diagnosis and guide treatment.
Medical imaging of the cervical spine
Sometimes, the clinical examination of the health professional is not enough to determine with conviction the pathology of the cervical spine.
In this case, the doctor will order a medical imaging test. It should be noted that these tests are not recommended immediately, because it has been noted that a dysfunction observed on medical imaging does not necessarily explain the patient's pain.
Here are the most common medical imaging tests prescribed by doctors:
- X-ray
- Scanner
- Cervical MRI
- EMG
When to worry
As mentioned previously, one of the main objectives during the physical (and radiological) examination is to exclude serious involvement of the cervical spine.
This includes in particular any systemic damage (such as cancer in the most serious cases), or damage to the spinal cord.
Here are the situations where a cervical spine injury would worry the medical profession. Often, they are emergencies, even going as far as surgery:
- Tingling, numbness and/or weakness in the arms, hands, legs or feet.
- Lack of coordination and difficulty walking
- Abnormal reflexes
- Muscle spasms
- Loss of sphincter control (urinary and fecal incontinence)
Available treatments
Fortunately, serious damage to the cervical spine is rare, and the vast majority of pathologies can be treated.
Often, the doctor is consulted in first intention following a neck pain. He can then refer to a competent therapist, or even a specialist for more complex cases.
In chronic cases, it should be noted that a multidisciplinary team where providers work as a team generally provides the best results.
Here are the most commonly used treatment modalities:
- Rest and cervical collar (in rare cases)
- Medication
- Physiotherapy (physiotherapy)
- Osteopathy
- Alternative medicine
- Homeopathy
- Infiltration
- Surgery
Conclusion
The cervical spine consists of the juxtaposition of cervical vertebrae serving in particular as support for the head, and allowing movement of the neck.
There are several pathologies related to the cervical spine. The symptoms will mainly depend on the irritated structure, as well as the level of inflammation.
A clinical and radiological examination will exclude serious damage requiring urgent medical intervention, and will clarify the diagnosis.
Treatments provided by healthcare professionals are generally effective in relieving pain and improving quality of life.
Good recovery !