Article reviewed and approved by Dr. Ibtissama Boukas, physician specializing in family medicine
Your doctor has diagnosed you with spinal stenosis (also called spinal canal narrowing, or narrow lumbar canal). Apparently, this could be the cause of your back pain.
What is spinal stenosis, and how does it manifest? Should we be worried (especially when all the forums seem to only talk about surgery!)? Is there a gentler treatment before considering the operation?
In the following article, we will discuss spinal stenosis in detail with an emphasis on a more 'natural' approach to relieving symptoms, and preventing your condition from getting worse.
Definition and Diagnosis of Spinal Stenosis
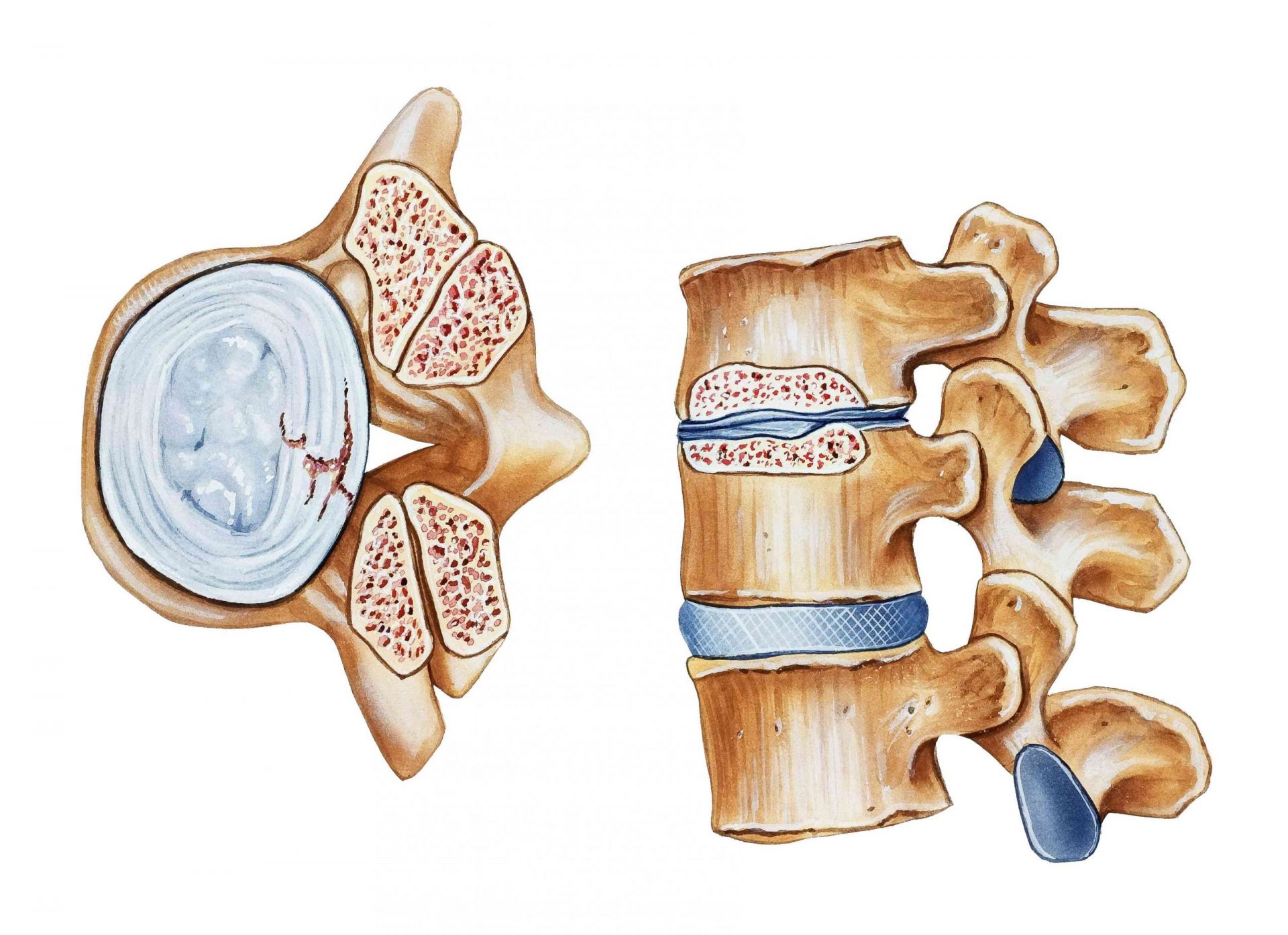
A mini anatomy lesson will help you better understand the diagnosis of spinal stenosis.
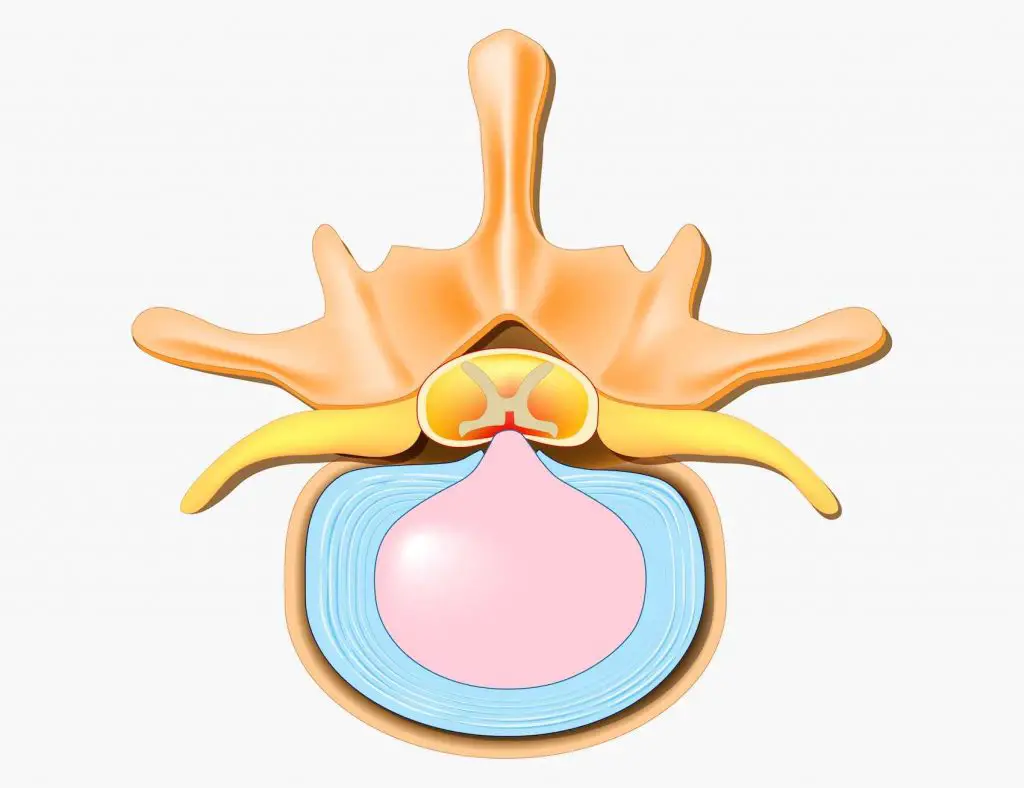
The spine (or spine) is composed of vertebrae superimposed. In the lumbar region (lower back), there are 5 vertebrae called L1, L2, L3, L4, and L5. There is a gap between each vertebrate called vertebral foramen.
The juxtaposition of the vertebrae (via the intervertebral discs and zygapophyseal joints) forms a channel called the spinal canal. This is where the spinal cord and from there that originate the nerve roots (which give for example the nerve sciatica or crural nerve).
In lumbar spinal stenosis, the size of this spinal canal decreases at the level of the lumbar vertebrae (L1 to L5). Normally this channel is about 15mm in diameter, but it is considered 'narrow' when it is less than 13mm.
But why does the channel narrow, you will ask me? The causes are multiple and depend on each individual. Here are the most common:
Vertebral osteoarthritis
Because it is often associated with osteophytes (bony prominences), osteoarthritis often results in a decrease in the size of the spinal canal. This degenerative cause is the most common of spinal stenosis. This is also the reason why the population concerned is often over 50 years old.
Spondylolisthesis
Le spondylolisthesis refers to a slipped vertebra. Inevitably, this will reduce the size of the spinal canal, and could lead to spinal stenosis.
Herniated disc
If the disc migrates backwards due to a herniated disc, it will reduce the size of the spinal canal and thus lead to spinal stenosis.
Congenital
As mentioned, the normal diameter of the vertebral foramen is about 15 mm. Some people are born with a smaller spinal foramen. They will therefore be more at risk of developing spinal stenosis in the future in the event of osteoarthritis or another condition that reduces the circumference of the spinal canal.
Other
Any pathology or condition that causes the spinal canal to shrink in size can lead to spinal stenosis. These include abscesses, infections, tumours, hematomas, yellow ligament hypertrophy, etc.
The diagnosis
Concretely, how can we differentiate between the various causes of spinal stenosis?
This is often the clinical examination and themedical imaging that will help determine the potential cause of spinal stenosis.
A doctor (or other back specialist) will perform a complete medical examination taking into consideration your medical history, and your associated conditions. Then he will do certain movements and other tests to identify the cause of your back problem.
Some imaging tests will help clarify the diagnosis. The X-ray will confirm the existence of spinal stenosis, and will determine if there is osteoarthritis or spondylolisthesis.
An MRI examination, on the other hand, will provide information on the integrity of nerve structures, discs, etc. An EMG might also be prescribed to better assess nerve conduction in the legs.
Anyway, the narrowing of the lumbar canal sometimes comes with its share of consequences, especially when we know the importance of the anatomical structures that pass through the spinal canal (such as the spinal cord, nerves, blood vessels, etc. .).
Spinal stenosis and cancer: what is the link?
Spinal stenosis can in rare situations be due to cancer. The latter can be primary, that is to say, originate directly in the spinal column or be secondary to a cancer occurring remotely and having caused spinal metastases.
Among the cancers implicated in spinal stenosis, we will cite:
- Osteochondroma
- Ewing's sarcoma
- Breast cancer
- Lung cancer
- Le prostate cancer
- kidney cancer
- Thyroid cancer
- Lymphoma
- Multiple myeloma
Primary or secondary spinal cancer can be diagnosed using multiple imaging tests, including:
- An x-ray of the spine: it makes it possible to analyze the state of the vertebrae and to highlight bone lysis or vertebral pinching that may suggest cancer.
- A computed tomography (CT) scan of the spine: this examination helps to observe not only the bony structures but also the adjacent structures. It makes it possible to highlight the bone masses in a direct and indirect way.
- Magnetic resonance imaging (MRI) of the spine: MRI helps to assess the impact of masses on non-osseous structures.
- Bone scintigraphy.
- A bone biopsy: it makes it possible to provide additional data concerning the characteristics of the tumor and to confirm its origin.
What are the symptoms of spinal stenosis?
What if I told you that spinal stenosis is sometimes asymptomatic? In fact, according to some studies, up to 28% people with a narrowed lumbar canal on medical imaging did not present with lumbar pain.
However, spinal stenosis often causes symptoms. This will depend on certain factors such as the narrowing itself, and also the irritated structures.
The most common symptom is lumbar pain (ache in the lower back). If the nerves are irritated, neurogenic symptoms such as sciatica ou cruralgia (such as radiating pain in the legs, tingling, numbness, etc).
In severe cases (qualified as severe spinal stenosis), we may be in the presence of a cauda equina syndrome.
Ponytail, what is it? These are nerve roots in the lower back that emerge from the spinal cord and provide control over the lower limbs and organs in the pelvic region.
At this time, we observe in particular anesthesia around the region of the genital organs, sphincter disorders (urinary and fecal incontinence), erectile dysfunction, or flaccid paralysis of the lower limbs. This is a medical emergency.
Another potential symptom of spinal stenosis is intermittent claudication. In addition to low back pain and pain in the lower limbs, the patient's complaints may be a feeling of heaviness in the legs, muscle fatigue and night cramps.
Typically, symptoms are worse on walking, and relieved on sitting. This comes from the fact that the lumbar flexion (as in a sitting position) momentarily increases the size of the lumbar canal, while extension and maintained lumbar lordosis (as in walking – especially when descending a slope) narrows it.
It's also why people with spinal stenosis find their symptoms ease when they lean on a shopping cart at the grocery store. This is the “Caddy sign”.
What is the treatment for spinal stenosis?
Treatment usually begins with so-called "conservative" methods to relieve the condition in a natural way. Unfortunately, some situations require more invasive interventions (we will come back to this). But in general, the treatment includes among others:
Medication
Although it does not correct the cause of spinal stenosis, medication can be helpful in controlling symptoms.
The doctor often starts with a prescription for anti-inflammatory, painkiller and/or muscle relaxants to control the initial symptoms.
In the case of neuropathic pain (for example, radiation in the leg associated with numbness and tingling), the doctor may prescribe anti-epileptics such as Lyrica.
In cases of severe pain, it is possible to resort to anti-depressants, oxycodone, codeine, morphine and its derivatives, etc.
Note: For more information on the choice of medication for his back pain, consult next article. On the other hand, know that it is imperative to follow the recommendations of your doctor. He will know how to choose the right drugs, and adjust the doses according to the medical history and the patient's condition.
Relative rest and lumbar corset
Please note, do not confuse relative rest and complete bed rest. The mistake many people with low back pain make is to stay in bed until the low back pain subsides.
Although it can relieve symptoms, this strategy comes with its share of consequences, such as increased stiffness, muscle atrophy, social isolation, and so on.
The best solution will therefore be to minimize rest as much as possible, and instead limit movements that accentuate the pain.
For example, a therapist might ask you to temporarily avoid swimming and other activities involving lumbar extension movements. Also, walking periods could be limited to a certain time so as not to aggravate the symptoms.
In more extreme cases, a doctor might prescribe a lumbar corset that would limit lumbar hyperlordosis. Again, don't get used to wearing the brace long term, and wear it more like a crutch that you would use after a sprained ankle.
Manual treatments and analgesic modalities
Since spinal stenosis is often accompanied by lower back pain, manual techniques from a therapist can help.
Massages or mobilizations from a osteopath, physiotherapist or chiropractor can reduce pain and reduce associated muscle tension.
On the other hand, these methods alone are not sufficient in the long term, and should ideally be accompanied by a active approach.
Active approach (kinesitherapy/physiotherapy)
It is sometimes difficult to conceive that exercise can help relieve back pain, especially when all movements are painful.
On the other hand, the scientific studies are unanimous: Physical activity is the best way to combat low back pain in the long term.
Of course, you have to be active in a safe and progressive way when you suffer from lower back pain, and the physiotherapist (physiotherapist) is the therapist of choice to guide you.
Useful exercises in the presence of spinal stenosis will be presented below.
Alternative treatments
Alternative treatments and natural products certainly have their place in the management of spinal stenosis, but their limits must first be identified.
No, an acupuncture session will not correct the source of your spinal stenosis. Nor even the cupping, Shiatsu-massage, medicinal plants, etc.
These modalities will rather act on the consequence of your spinal stenosis (such as pain and/or lumbar stiffness), and offer you often temporary relief.
If the pain prevents you from going about your business, and you prefer to limit the intake of medication, these treatments can be effective in addition to a medical approach to improve your quality of life.
Other forms of alternative medicine used in the treatment of spinal stenosis include:
- acupressure mat
- myotherapy
- Quinton plasma
- percutaneous hydrotomy
- therapeutic yoga
- craniosacral therapy
Adaptation of the workstation
Certain professional activities inevitably involve risks for the back. We are thinking, among others, of delivery people, cleaning ladies, truck drivers, etc.
In other words, tasks involving repetitive motions, heavy lifting, and/or prolonged static postures can increase back pain.
If your symptoms seem to get worse after a day at work, a job adaptation could help.
Un Occupational therapist is the professional of choice to adjust your screens, show you optimal load handling techniques, propose a gradual return plan after a shutdown, etc.
In extreme cases, the retraining can even be considered.
Infiltrations
The doctor may suggest infiltrations to relieve the pain, especially when the medication does not seem to have an effect.
In general, the doctor goes for a cortisone infiltration at the lumbar level (depending on the levels and irritated structures)
The ideal would be to use a ultrasound-guided infiltration to maximize results.
Are there exercises to do?
As mentioned previously, a kinesitherapist (physiotherapist) could prescribe therapeutic exercises aimed at relieving you and preventing the aggravation of your condition.
If you have spinal stenosis, lumbar extension movements may make your symptoms worse, and flexion movements (like bending forward) may provide relief.
This is because lumbar flexion momentarily increases the diameter of the lumbar canal, while lumbar extension narrows it.
En Mckenzie method, we will then say that your preferred direction is lumbar flexion.
If so, your therapist might give you postural tips to actively reduce lumbar lordosis (especially if arching your back increases your symptoms).
He might also prescribe bending exercises such as those mentioned below. To this will be added a lumbar stabilization program aimed at toning the muscles of the trunk to protect the lumbar region.
Obviously, these exercises will be adapted to your condition, and integrated into a global approach.
Exercise 1: Posterior pelvic tilt
- Lie on your back with your knees bent
- Tilt the pelvis backwards so as to flatten your lumbar region against the floor.
- Hold the position for 3 seconds and return to the initial position
- Repeat 15 times, taking breaks as needed.
Exercise 2: Repeated Mckenzie Bend Squats
- Lie on your back and bend your knees
- Bring the knees towards your shoulders at the same time, and add a 3 second overpressure with your hands (as if you were giving yourself a hug!). Then return to the initial position.
- Repeat 15 times, taking breaks as needed.
Exercise 3: Repeated McKenzie Squats
- Sit in a chair with your legs apart
- Lean your trunk so that your arms are as far back as possible (between your legs). Hold for 3 seconds in the fully flexed position and then return to the starting position.
- Repeat 15 times, taking breaks as needed.
Exercise 4: Sit-ups
- Lie on your back and bend your knees. Place hands against you as shown.
- In the same movement, take your shoulder blades off the ground and bring your elbows towards your knees. You will feel a contraction of the abdominals that you will have to hold for 3 seconds without blocking your breathing.
- Do 2 sets of 10 reps.
Exercise 5: Abs Swiss ball
- Lie on your back and place a Swiss ball between your knees and arms as shown.
- In the same movement, squeeze the Swiss ball by bringing your arms and legs against each other. Hold the contraction for 5 seconds.
- Repeat 15 times, taking breaks as needed.
Note: These exercises are not worth a medical consultation. Be sure to exhale on exertion, and stop as soon as you feel persistent pain. If in doubt, consult a healthcare professional.
How to sleep?
It is not uncommon for people diagnosed with spinal stenosis to complain of poor quality sleep.
With this in mind, here are some sleeping postures that are sometimes effective in relieving symptoms and sleep better at night.
Lying on your back with a pillow under your knees
This position reduces the anteversion of the pelvis (lumbar hyperlordosis), which reduces stress on the facet joints. Basically, keeping your knees slightly bent will prevent your back from arching excessively, reducing the stress on your vertebrae.
For people who see their symptoms worsen in extension (often the case in the presence of spinal stenosis), this position can be comfortable and thus improve the quality of sleep.
Lying on your side with a pillow between your legs
Keeping a pillow between the legs reduces lumbar torsion. By bending the knees, this also decreases lumbar lordosis (sometimes painful in the presence of spinal stenosis).
For added comfort, many of my patients opt for a knee pillow such as this one.
When to consider surgery?
Unfortunately, some people diagnosed with spinal stenosis will need resort to the operation to relieve their symptoms.
Remember that this treatment option should not be considered out of hand. On the other hand, surgery will be considered in the following situations:
Red flags
Some conditions require urgent medical (and often surgical) intervention. This is particularly the case of the cauda equina syndrome discussed above.
Symptoms are often severe and disabling.
Persistence of pain
Sometimes spinal stenosis causes a persistent functional disability. In other words, it greatly affects the quality of life of the sufferer.
In the event of persistent disability (between 3 and 6 months) despite well-conducted conservative treatment, a medical specialist may consider the surgical option.
What types of surgeries are available?
Once the doctor has decided that surgery is the preferred option for treating spinal stenosis, the goal will be to increase the size of the spinal canal. This means correcting (or removing) structures that narrow the spinal canal.
When indicated, surgery for spinal stenosis (cervical or lumbar) is based on more or less complex surgical techniques, the most frequently used of which are:
- La Decompression Laminoplasty
- arthrodesis
- La discectomy
- La corpectomy
- Foraminotomy
- La flavectomy
Obviously, an orthopedic surgeon will discuss with his patient the types of surgery possible, the associated risks, the prognosis for recovery, etc.
Recovery from spinal stenosis surgery
In general, in the event of hospitalization scheduled for surgery, patients only stay one to two days following the operation.
Wearing a cervical collar is generally not recommended by doctors in case of laminoplasty. However, wearing a neck brace flexible is desirable in some patients, in particular to better support the spine during the first days following the procedure.
Regarding the duration of hospitalization, this can range from 24 to 48 hours, in the absence of postoperative complications. The patient is allowed to get out of bed and start walking from the first day after the procedure.
The first bandage is redone 24 h after the operation, then repeat every other day until the wound is completely healed.
At the end of 6 weeks of the intervention, the patient must make his first postoperative consultation then a second one after 3 months of the intervention. The consultation of the 3rd month will be based on the clinical and radiological control serving to evaluate the evolution of the intervention. If the pain persists, the doctor may recommend additional follow-up time.
45 days after the operation, the patient can contact a physiotherapist to benefit from the sessions physiotherapy can be based on gentle massages full muscles or alternatively Stretching. However, the physio should be gradual and gentle for faster and more effective recovery. However, other sporting activities should be resumed in the long term (from the first months) provided that any sudden physical effort or the carrying of heavy loads is avoided.
In the event of the appearance of new symptoms or usual symptoms such as shooting pains, numbness, muscle weakness or paralysis, you should never hesitate to report them to your surgeon or doctor.
Conclusion
So much for spinal stenosis! Hopefully you are now more familiar with this condition if your doctor ever gave you this diagnosis.
More precisely, you have an idea of the different possible causes of spinal stenosis, and also have knowledge of the symptoms according to the anatomical structures affected.
As for the treatment, remember that it should start with so-called conservative methods with the aim of avoiding surgery as much as possible. Passive treatments can relieve you, but don't forget to complement them with an active approach.
In extreme cases, surgery remains a viable option. An orthopedist will know how to weigh the pros and cons of surgery based on the symptoms and their implication in the patient's life.
Good recovery!